Perioscopic Micro Gum Rejuvenation (PMGR)
A Newer Method Using A Dental Endoscope
Can Help Avoid Gum Surgery
For the last 75 years, we have accepted BLIND cleaning as the standard, whether regular dental cleanings or deep cleanings. Even the best hygienist will leave 30-50% tartar behind in deep pockets. NOW THE GAME HAS CHANGED. Perioscopy allows us to ACTUALLY SEE what we are instrumenting for the first time.
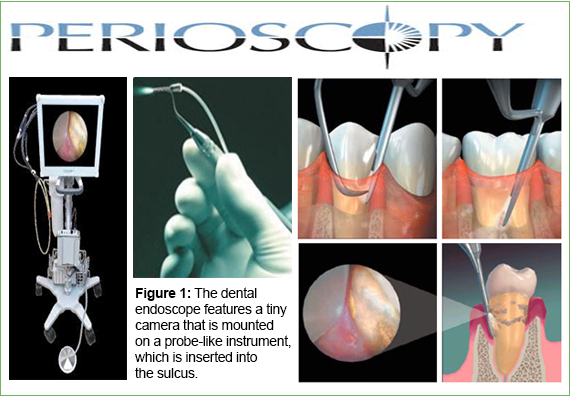
1. The dental endoscope provides a magnified view, up to 48 times, of the subgingival area and root. A tiny camera is mounted on a probe-like instrument that inserts into the gingival sulcus. Aided by intense fiber-optic lighting and continual flushing of the pocket with water, the endoscope displays magnified images of the root surface on a video screen. Detailed images of crown margins, subgingival decay, furcations, and embedded calculus with adjacent inflamed tissue are visible.
2. The dental endoscope reveals that significant calculus remains on the root after closed debridement (30-50%) that is not detectable with an explorer. This calculus contains lacuna that harbor microorganisms, including bacteria that initiate periodontal infections. Removal of bacteria-laden calculus is conducive to healing and should remain the primary goal of periodontal instrumentation. Failure to remove undetected calculus impedes healing of the pocket, resulting in the need for further root planing or periodontal surgery.
3. Another common myth is that the smoothness of roots (felt with an explorer, probe, or curet) means they are calculus free. The dental endoscope clearly illustrates that calculus is missed following closed procedure scaling. It can be microscopically embedded into the root and, therefore, undetectable by an explorer. Restorations, crown margins, cementoenamel junctions, grooves, and depressions are other areas that commonly harbor calculus dismissed as roughness. The feeling of smoothness is not an accurate predictor of calculus removal.
4. Periodontal practices regularly receive referrals from general dental offices because of residual pocket depth with bleeding, following root planing procedures. With no fault of the hygienist, BLIND CLEANING IS FLAWED (30-50% left behind). With the use of a dental endoscope, the cause of these residual pockets, usually calculus, can be seen and removed. Pocket reduction occurs once calculus is thoroughly removed. Thus, many patients not all can benefit from Perioscopy and not need to be referred to a periodontist for more extensive procedures like gum surgery. One study showed that 71 of 73 patients who were diagnosed as needing gum surgery did not need gum surgery after perioscopy treatment.
How long does Perioscopy take?
Perioscopy experienced clinicians can typically provide therapy in a similar time frame as clinicians providing "blind instrumentation". Becoming proficient in dental endoscopy requires training, patience and practice.
Generally, we find the entire mouth can be cleaned in 2 sessions (11/2-2hrs per session). This can vary depending on each case. Sometimes, It may require 4 sessions (1-1/2hrs per session)
Does it hurt?
Dental endoscopy is provided under local anesthesia to ensure patient comfort.
What can your patients expect?
Many times, deep pockets improve significantly, although each patient may respond differently. Independent studies have shown that Perioscopy technology provided by experienced clinicians demonstrate improved patient treatment outcomes.
How long has your office been doing this treatment?
Before I answer this question, I must give kudos to a few people. Perioscopy has been around since 2001. Dr. John Kwan of Berkeley revived the technology by carrying the technology and fabricating the current version we now use. Thank you, Dr. Kwan. Lynn Groff kindly gave our special dental hygienists valuable training in perioscopy.
Judy Carroll of Periopeak.com has helped our special dental hygienists learn her proven results since 2001 of her treatment protocol. She is one special person and totally dedicated to helping improve patients’ lives. Our office is grateful to her.
I believe no matter what protocol you choose, and everyone has their own way of doing things, there is no better way to treat gum disease than with perioscopy. We have been using the latest version of the Perioscopy unit for about 5 years. In that time, we drastically modified our technique. Our office has realized that just because you buy a unit and use it, there is no guarantee of good results. It takes a tremendous amount of research, gaining knowledge and time to modify and improve the delivery of care.
As we all know, there is such a huge connection between how the health of the mouth can influence your overall bodily health. We are constantly studying and learning to help improve our ability to help our patients. We are ADVANCING DENTISTRY BEYOND THE MOUTH.

